Abstract
Objective
To observe the effect of Mo-Rubbing abdomen manipulation on glucose metabolism and inflammatory factors in rats with type 2 diabetes mellitus (T2DM).
Methods
Sixty Sprague-Dawley rats were randomly divided into a normal group (n=10) and a group for modeling (n=50) using the random number table method. Rats in the group for modeling were induced to form T2DM models by a high-sugar and high-fat diet combined with intraperitoneal injection of streptozotocin. Thirty successfully modeled rats were randomly divided into a model group, a Mo-Rubbing abdomen group, and a metformin group, with 10 rats in each group. Rats in the normal group and the model group received no intervention, those in the Mo-Rubbing abdomen group received Mo-Rubbing abdomen manipulation, and those in the metformin group received metformin by gavage. After 8-week intervention, fasting insulin (FINS), fasting plasma glucose (FPG), homeostasis model assessment for insulin resistance (HOMA-IR) and area under the curve at the oral glucose tolerance test (AUC-OGTT), as well as serum inflammatory factors interleukin (IL)-1β, IL-6, and tumor necrosis factor (TNF)-α were detected, and the morphological changes of the pancreas were also observed.
Results
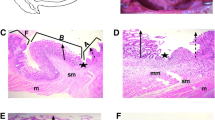
After the 8-week intervention, the levels of FINS, FPG, HOMA-IR, and AUC-OGTT of rats in the Mo-Rubbing abdomen group were significantly lower than those in the model group (P<0.05); the pancreatic injury degree in the Mo-Rubbing abdomen group and the metformin group was lower than that in the model group. Compared with the model group, the serum IL-1β, IL-6, and TNF-α levels of rats in the Mo-Rubbing abdomen group were significantly decreased (P<0.05), and the serum IL-1β and TNF-α levels of the metformin group showed a downward trend; the serum IL-6 and TNF-α levels in the Mo-Rubbing abdomen group were significantly lower than those in the metformin group (P<0.01). There was a significant positive correlation between FPG with IL-1β, IL-6, and TNF-α in the T2DM rats (P<0.01).
Conclusion
Mo-Rubbing abdomen manipulation reduces the inflammatory response and improves the morphological changes of the pancreas in T2DM rats, thereby achieving the effect of lowering blood glucose.
摘要
目的
观察摩腹对 2 型糖尿病(T2DM)大鼠糖代谢和炎症因子的影响.
方法
将 60 只Sprague-Dawley大鼠采用随机数字表法分为**常组(n=10)和造模组(n=50). 造模组采用高糖高脂饲料联合腹腔注射链脲佐菌素诱导大鼠形成T2DM模型. 将造模成功的30 只大鼠再随机分为模型组、 摩腹组和二甲双胍组, 每组 10 只. **常组和模型组不干预, 摩腹组予以摩腹, 二甲双胍组予以二甲双胍灌胃. 干预 8 周后测定各组空腹胰岛素(FINS)、 空腹血糖(FPG)、 稳态模型的胰岛素抵抗指数(HOMA-IR)和口服葡萄糖耐量试验曲线下面积(AUC-OGTT), 检测血清炎症因子白细胞介素(IL)-1β、 IL-6 和肿瘤坏死因子(TNF)-α, 同时观察胰腺形态学变化.
结果
干预 8 周后, 摩腹组大鼠FINS、 FPG、 HOMA-IR和AUC-OGTT均显著低于模型组(P<0.05); 摩腹组和二甲双胍组胰腺损伤程度均小于模型组. 与模型组比较, 摩腹组大鼠血清IL-1β、 IL-6 和TNF-α含量均显著下降(P<0.05), 二甲双胍组大鼠血清IL-1β和TNF-α含量均呈下降趋势; 摩腹组血清IL-6 和TNF-α显著低于二甲双胍组 (P<0.01). T2DM大鼠FPG与IL-1β、IL-6 和TNF-α均呈显著**相关(P<0.01).
结论
摩腹能够降低T2DM大鼠炎症反应, 改善胰腺的形态学变化, 从而达到降低血糖的效果.
Similar content being viewed by others
References
YU S, CHENG Y, ZHANG L, YIN Y, XUE J, LI B, GONG Z, GAO J, MU Y. Treatment with adipose tissue-derived mesenchymal stem cells exerts anti-diabetic effects, improves long-term complications, and attenuates inflammation in type 2 diabetic rats. Stem Cell Res Ther, 2019, 10(1): 333.
NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in diabetes since 1980: a pooled analysis of 751 population-based studies with 4.4 million participants. Lancet, 2016, 387(10027): 1513–1530.
WANG W, ZHANG J, WANG H, WANG X, LIU S. Vitamin D deficiency enhances insulin resistance by promoting inflammation in type 2 diabetes. Int J Clin Exp Pathol, 2019, 12(5): 1859–1867.
REINEHR T, ROTH C L. Inflammation markers in type 2 diabetes and the metabolic syndrome in the pediatric population. Curr Diab Rep, 2018, 18(12): 131.
LIU H Q, QIU Y, MU Y, ZHANG X J, LIU L, HOU X H, ZHANG L, XU X N, JI A L, CAO R, YANG R H, WANG F. A high ratio of dietary n-3/n-6 polyunsaturated fatty acids improves obesity-linked inflammation and insulin resistance through suppressing activation of TLR4 in SD rats. Nutr Res, 2013, 33(10): 849–858.
KHAN R M M, CHUA Z J Y, TAN J C, YANG Y, LIAO Z, ZHAO Y. From pre-diabetes to diabetes: diagnosis, treatments and translational research. Medicina (Kaunas), 2019, 55(9): 546.
KARSTOFT K, PEDERSEN B K. Exercise and type 2 diabetes: focus on metabolism and inflammation. Immunol Cell Biol, 2016, 94(2): 146–150.
DONATH M Y. Targeting inflammation in the treatment of type 2 diabetes: time to start. Nat Rev Drug Discov, 2014, 13(6): 465–476.
REHMAN K, AKASH M S H, LIAQAT A, KAMAL S, QADIR M I, RASUL A. Role of interleukin-6 in mellitus. Crit Rev Eukaryot Gene Expr, 2017, 27(3): 229–236.
GBD 2015 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet, 2016, 388(10053): 1545–1602.
ZHANG X, CAO D, YAN M, LIU M. The feasibility of Chinese massage as an auxiliary way of replacing or reducing drugs in the clinical treatment of adult type 2 diabetes: a systematic review and meta-analysis. Medicine (Baltimore), 2020, 99(34): e21894.
DOLO P R, HUANG K, WIDJAJA J, LI C, ZHU X, YAO L, HONG J. Distal gastric mucosa ablation induces significant weight loss and improved glycemic control in type 2 diabetes Sprague-Dawley rat model. Surg Endosc, 2020, 34(10): 4336–4346.
LI Y J, WANG C Y, REN X R, WANG Y C, ZHU H F. Effects of glibenclamide on AGEs/RAGE/NF-κB pathway and placental dysfunction in gestational diabetes mellitus rats. Zhongguo Yousheng Yu Yichuan Zazhi, 2021, 29(3): 339–344.
MANELL H, STAAF J, MANUKYAN L, KRISTINSSON H, CEN J, STENLID R, CIBA I, FORSLUND A, BERGSTEN P. Altered plasma levels of glucagon, GLP-1 and glicentin during OGTT in adolescents with obesity and type 2 diabetes. J Clin Endocrinol Metab, 2016, 101(3): 1181–1189.
ICHIKAWA R, TAKANO K, FUJIMOTO K, MOTOMIYA T, KOBAYASHI M, KITAMURA T, SHICHIRI M. Basal glucagon hypersecretion and response to oral glucose load in prediabetes and mild type 2 diabetes. Endocr J, 2019, 66(8): 663–675.
DAI C G, CHEN G, YANG J J, CHEN M, QIN J J, ZHU W F. Effects of acupoint massage and sitagliptin on adiponectin and irisin in obese patients with type two diabetes mellitus. **bu Zhongyiyao, 2020, 33(7): 45–48.
WANG W H, ZHANG R. Chinese medicine combined with abdominal massage in the treatment of type 2 diabetes mellitus with abdominal obesity. Zhongxiyi Jiehe **nxueguanbing Dianzi Zazhi, 2018, 6(34): 184–185.
HOLST S, LUND I, PETERSSON M, UVNÄS-MOBERG K. Massage-like stroking influences plasma levels of gastrointestinal hormones, including insulin, and increases weight gain in male rats. Auton Neurosci, 2005, 120(1–2): 73–79.
BERMINGHAM-MCDONOGH O, RUBEL E W. Hair cell regeneration: winging our way towards a sound future. Curr Opin Neurobiol, 2003, 13(1): 119–126.
YUAN H, SILBERSTEIN S D. Vagus nerve and vagus nerve stimulation, a comprehensive review: part I. Headache, 2016, 56(1): 71–78.
BONAZ B, SINNIGER V, PELLISSIER S. Vagus nerve stimulation at the interface of brain-gut interactions. Cold Spring Harb Perspect Med, 2019, 9(8): a034199. development of insulin resistance and type 2 diabetes
BONAZ B, SINNIGER V, PELLISSIER S. Anti-inflammatory properties of the vagus nerve: potential therapeutic implications of vagus nerve stimulation. J Physiol, 2016, 594(20): 5781–5790.
PEDERSEN B K. Anti-inflammatory effects of exercise: role in diabetes and cardiovascular disease. Eur J Clin Invest, 2017, 47(8): 600–611.
REMPEL J D, PACKIASAMY J, DEAN H J, MCGAVOCK J, JANKE A, COLLISTER M, WICKLOW B, SELLERS E A. Preliminary analysis of immune activation in early onset type 2 diabetes. Int J Circumpolar Health, 2013, 72: 21190.
IBARRA URIZAR A, FRIBERG J, CHRISTENSEN D P, LUND CHRISTENSEN G, BILLESTRUP N. Inflammatory cytokines stimulate bone morphogenetic protein-2 expression and release from pancreatic beta cells. J Interferon Cytokine Res, 2016, 36(1): 20–29.
SMITKA K, MAREŠOVÁ D. Adipose tissue as an endocrine organ: an update on pro-inflammatory and anti-inflammatory microenvironment. Prague Med Rep, 2015, 116(2): 87–111.
FENG W. The influence of abdominal massage on expression of IL-1, Caspase-3 and Bcl-2 in pancreas of type 2 diabetic rats. Anmo Yu Kangfu Yixue, 2019, 10(13): 47–49.
VAN OPDENBOSCH N, LAMKANFI M. Caspases in cell death, inflammation, and disease. Immunity, 2019, 50(6): 1352–1364.
AN Y, ZHANG H, WANG C, JIAO F, XU H, WANG X, LUAN W, MA F, NI L, TANG X, LIU M, GUO W, YU L. Activation of ROS/MAPKs/NF-κB/NLRP3 and inhibition of efferocytosis in osteoclast-mediated diabetic osteoporosis. FASEB J, 2019, 33(11): 12515–12527.
ALNAHDI A, JOHN A, RAZA H. Augmentation of glucotoxicity, oxidative stress, apoptosis and mitochondrial dysfunction in HepG2 cells by palmitic acid. Nutrients, 2019, 11(9): 1979.
SONG W, WEI L, DU Y, WANG Y, JIANG S. Protective effect of ginsenoside metabolite compound K against diabetic nephropathy by inhibiting NLRP3 inflammasome activation and NF-κB/p38 signaling pathway in high-fat diet/streptozotocin-induced diabetic mice. Int Immunopharmacol, 2018, 63: 227–238.
CORTEZ-NAVARRETE M, MARTÍNEZ-ABUNDIS E, PÉREZ-RUBIO K G, GONZÁLEZ-ORTIZ M, MÉNDEZ-DEL VILLAR M. Momordica charantia administration improves insulin secretion in type 2 diabetes mellitus. J Med Food, 2018, 21(7): 672–677.
SAHA S, SCHWARZ P E, BERGMANN S, BORNSTEIN S R, GRAESSLER J, KOPPRASCH S. Circulating very-low-density lipoprotein from subjects with impaired glucose tolerance accelerates adrenocortical cortisol and aldosterone synthesis. Horm Metab Res, 2013, 45(2): 169–172.
Acknowledgments
This work was supported by the Second Batch of Scientific Research Project of the National TCM Clinical Research Base of the State Administration of Traditional Chinese Medicine (国家中医药管理局国家中医临床研究基地业务建设第二批科研专项课题, No. JDZX2015127); Postgraduate Research & Practice Innovation Program of Jiangsu Province (江苏省研究生培养创新工程研究生科研与实践创新计划, No. KYCX20_1538); Undergraduate Innovation and Entrepreneurship Training Program of Jiangsu Province (江苏省大学生创新创业训练计划, No. 201910315071Y).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that there is no potential conflict of interest in this article.
Additional information
Statement of Human and Animal Rights
The treatment of animals conformed to the ethical criteria in this experiment.
First Author: XIE Zhouyu, master degree candidate
Rights and permissions
About this article
Cite this article
**e, Z., Xu, J., Kong, X. et al. Effects of Mo-Rubbing abdomen manipulation on glucose metabolism and inflammatory factors in rats with type 2 diabetes mellitus. J. Acupunct. Tuina. Sci. 20, 354–362 (2022). https://doi.org/10.1007/s11726-022-1336-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11726-022-1336-2
Keywords
- Tuina
- Massage
- Mo-Rubbing Manipulation
- Diabetes Mellitus, Type 2
- Inflammatory Factors
- Carbohydrate Metabolism